生物电阻抗分析:BIA如何测量身体成分
生物电阻抗分析(或BIA)是一种简单且无创的测试,通过电极测量低电压电流如何在身体中循环。

BIA:评估身体成分的一种方法
因为BIA有助于区分身体脂肪、肌肉和体水在您身体组织中的分布情况, 它被广泛用于确定您的身体成分。 当脂肪相对于瘦体重过多时,这被称为“身体成分改变。” 尽管许多人只关注体重,但已知身体成分的改变会增加患各种疾病的风险,包括心血管疾病、2型糖尿病和高血压。 因此,BIA可以是对您健康的关键评估。这是您应该了解的关于BIA方法、历史、准确性和潜在偏差的信息。
什么是生物电阻抗分析?
生物电阻抗分析(BIA),或生物阻抗,是 t生物组织对低电压电流流动的电阻测量。
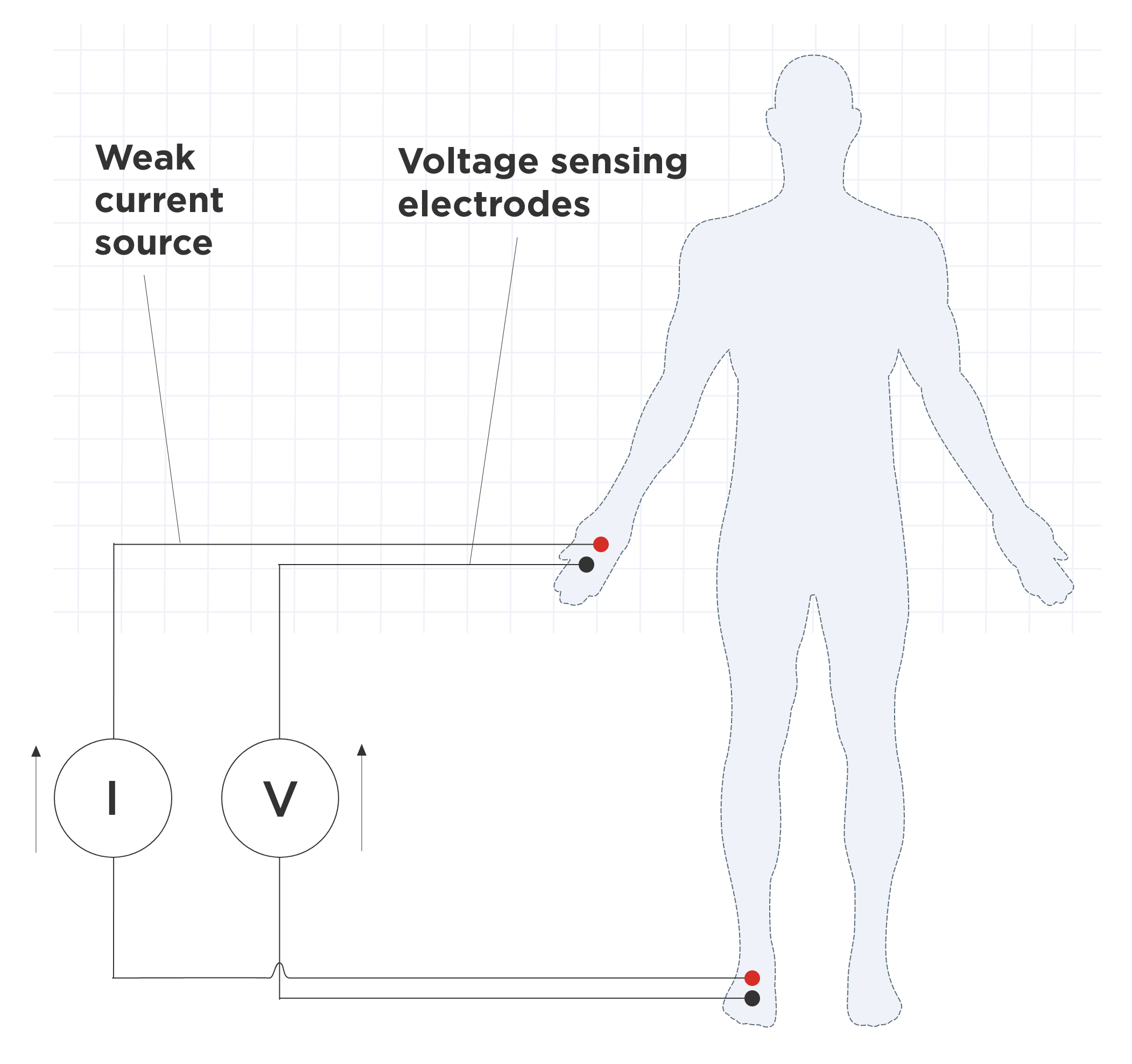
人体由不同类型的组织组成,这些组织具有不同水平的电导率。电压约为70微安(μA)时,电流主要通过导电性最强的组织,如水或肌肉。
通过测量源电极和接收电极之间的电压降,BIA 确定这些组织对电流通过的阻力水平。
称为“阻抗”,这resistance(Z)对应于 的比率电压 (V) 在与组织接触的两个点之间测量,强度 (I) of the frequency to the current applied to this tissue.
阻抗计算公式为 Z=V/I。
生物电阻抗分析从何而来?
虽然最早的电阻抗测试可以追溯到乔治·西蒙·欧姆(1788-1854),但其在人体和生物组织测量中的应用是在20世纪下半叶被理论化的。
1962年, 在a paper entitled "组织的生物电特性。临床医学中的阻抗测量". 曲线的重要性,法国医生Thomasset首次引入了一种使用两个电极的方法,通过比较两个电流频率,使任何医生都能计算出瘦体重,并获得患者营养状况的满意估计。
With time and a growing interest in body composition, other methods emerged. In 1994, the National Institutes of Health (NIH) agreed on a technology assessment, whose purpose was to "provide physicians with a responsible assessment of bioelectrical impedance analysis (BIA) technology for body composition measurement (源)。
生物电阻抗分析如何指示身体成分?
生物电阻抗分析现在广泛应用于医学领域,以区分体内的水分、体脂和骨骼肌的数量。
分析首先获得总身体水分(TBW)。这是可以在体内和体外细胞中找到的液体量。对于成年人来说,总身体水分代表 45到60%的体重总量。
其他成分——具有更多绝缘特性的成分,如体脂或皮肤——将更“有阻力”,这意味着它们导电效果较差。
使用在不同频率下测量的生物电阻抗比率,复杂的方程式随后估算出体内的无脂肪质量。最后,从总重量中扣除体脂量。
身体成分之外
注意:生物电阻抗也是心脏病学中用于评估的方法脉搏波速度, 另一种生物标志物,用于确定动脉的硬度以推断心血管健康。
脂肪组织中的电阻测量
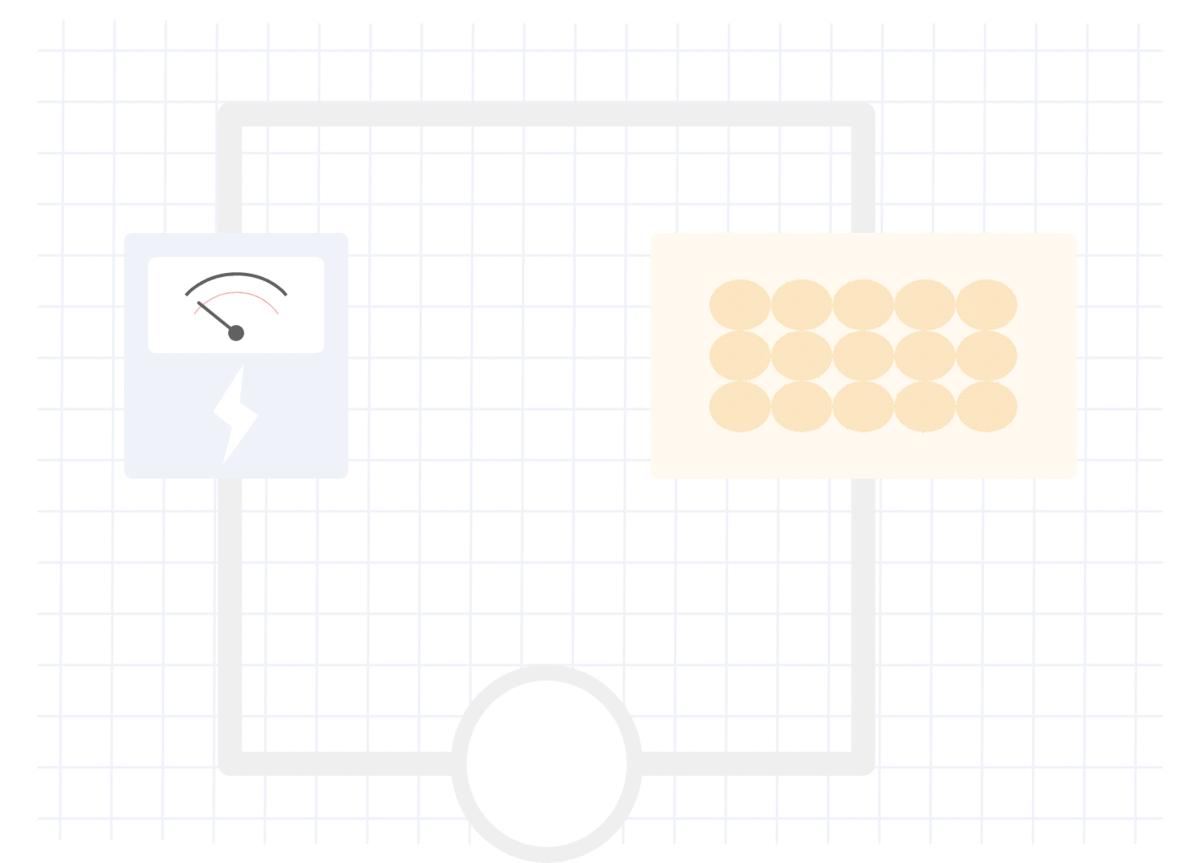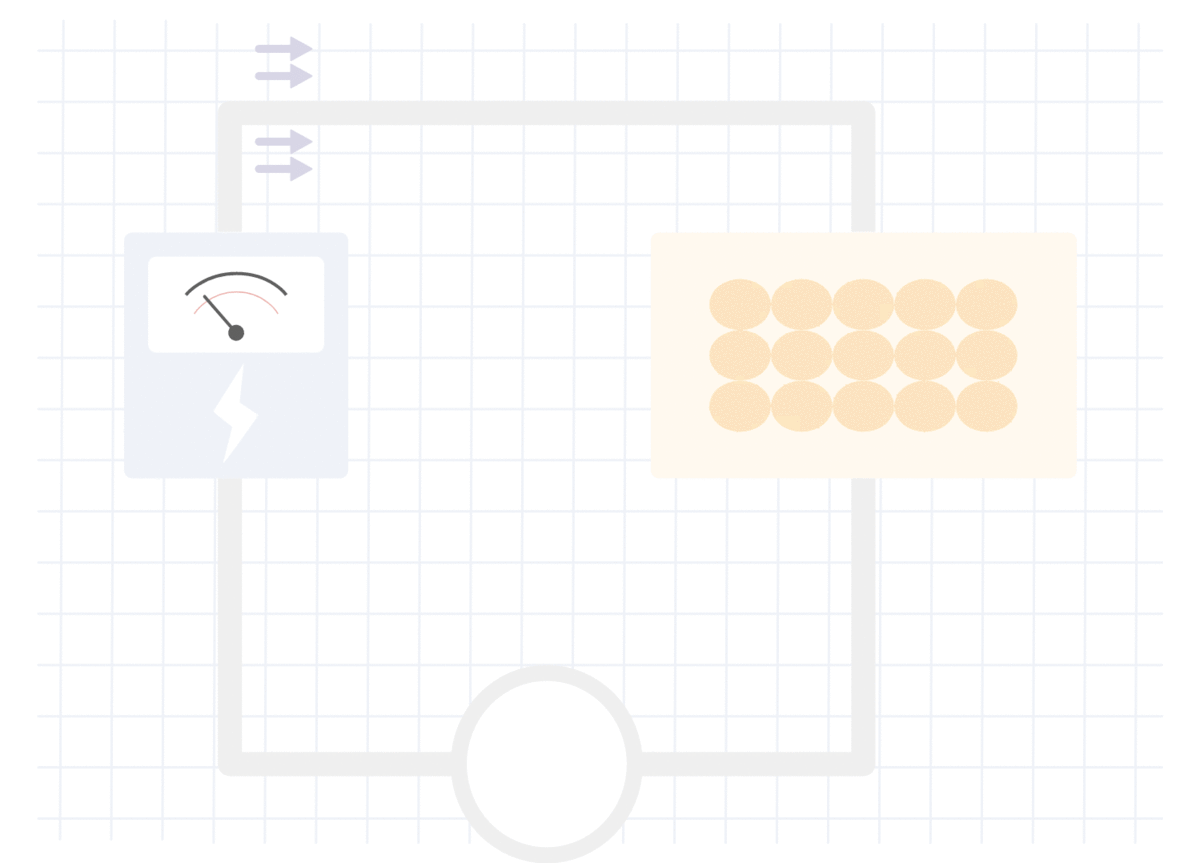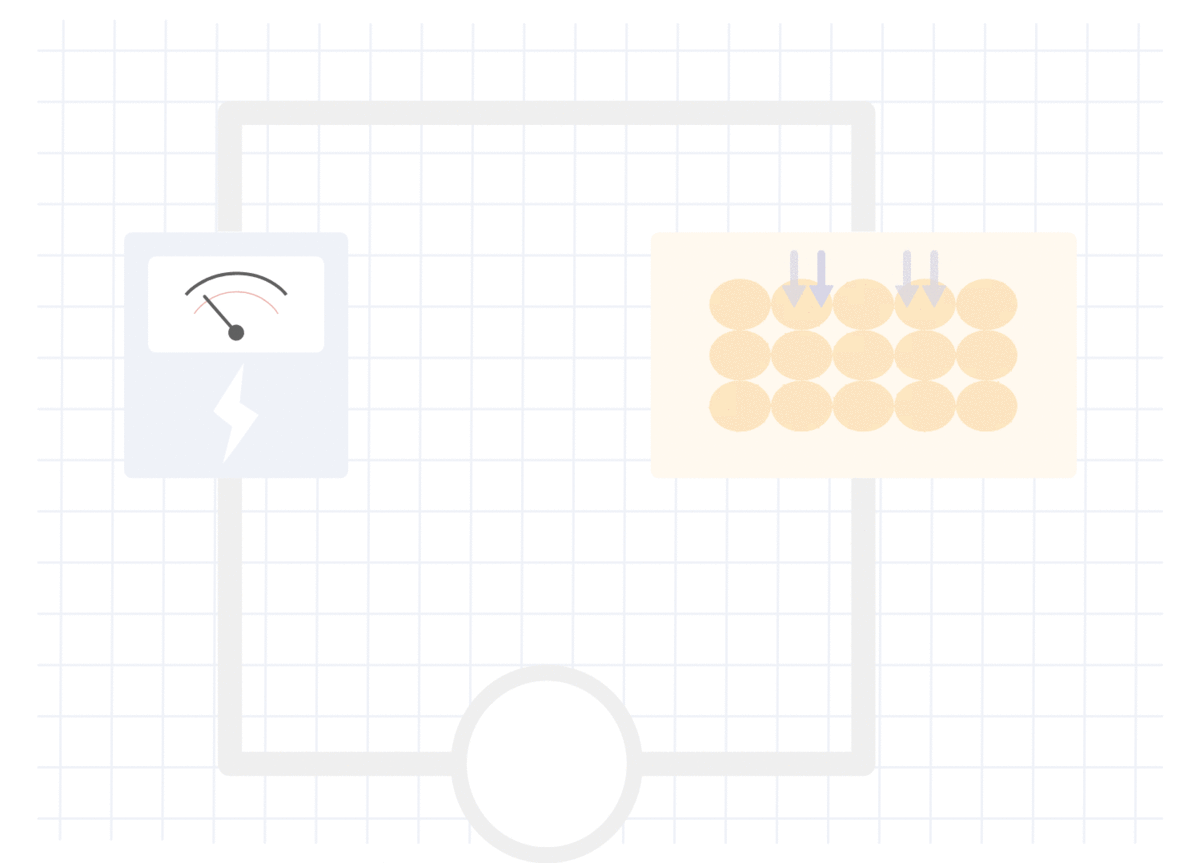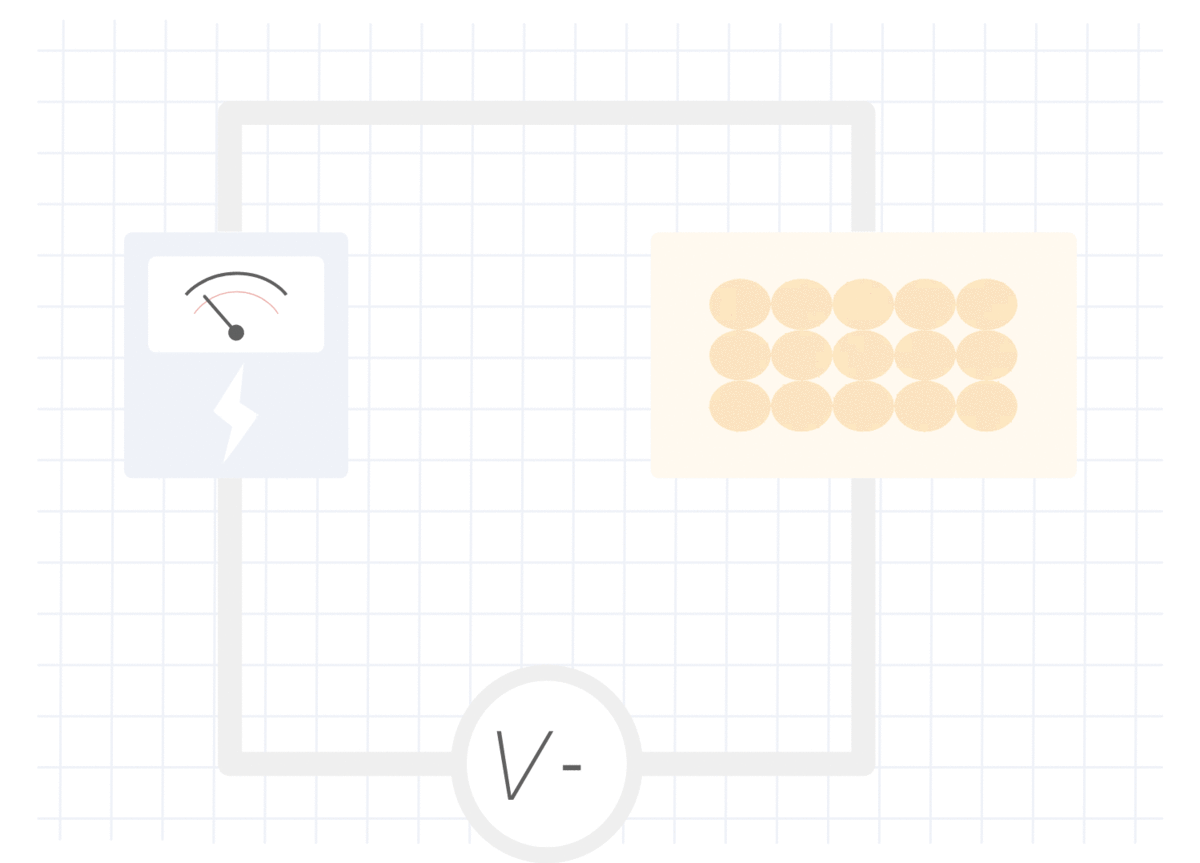
在无脂组织中测量的电阻
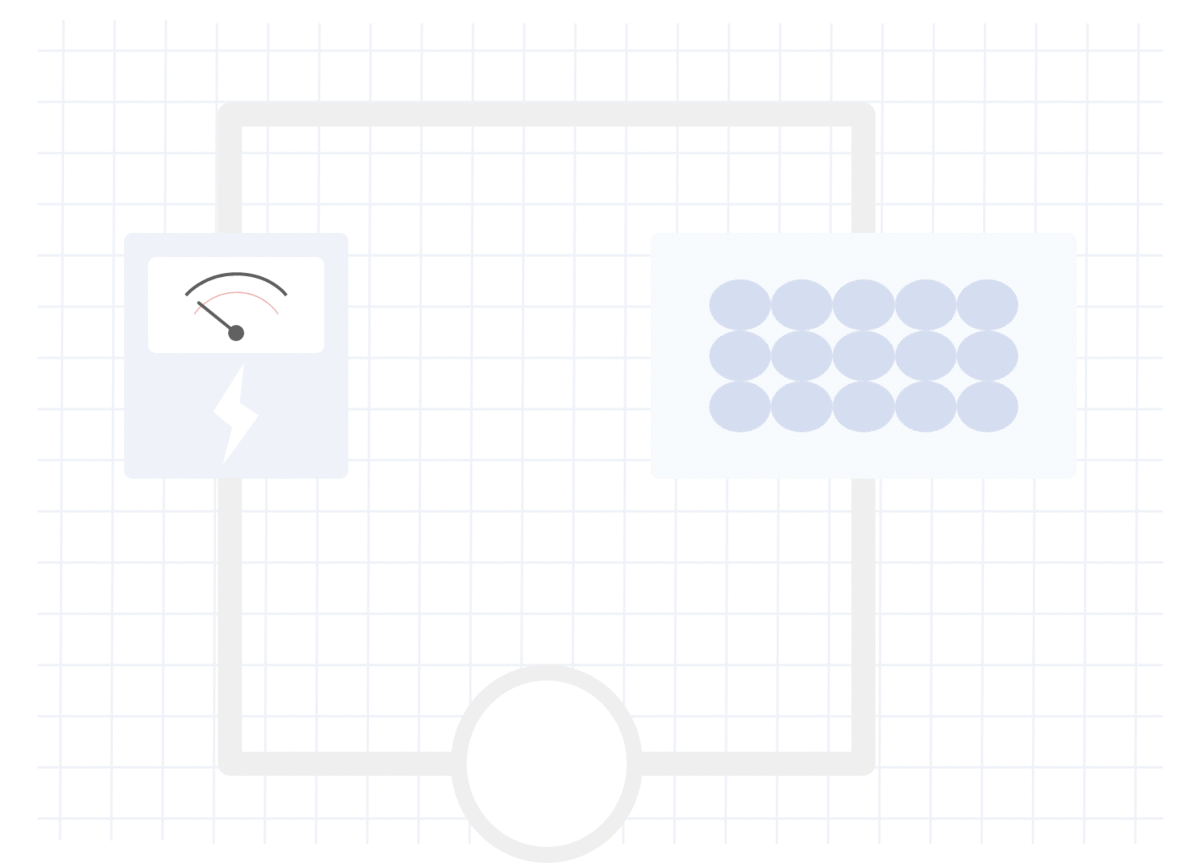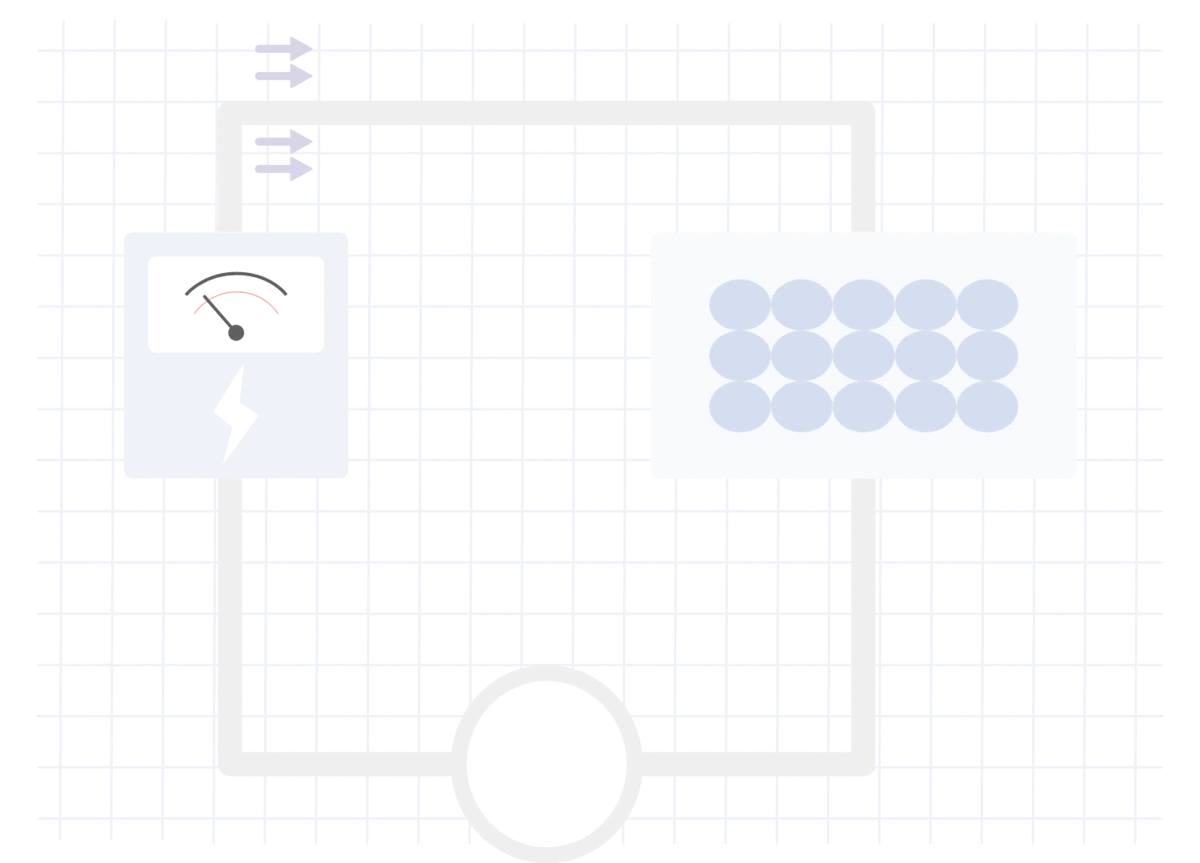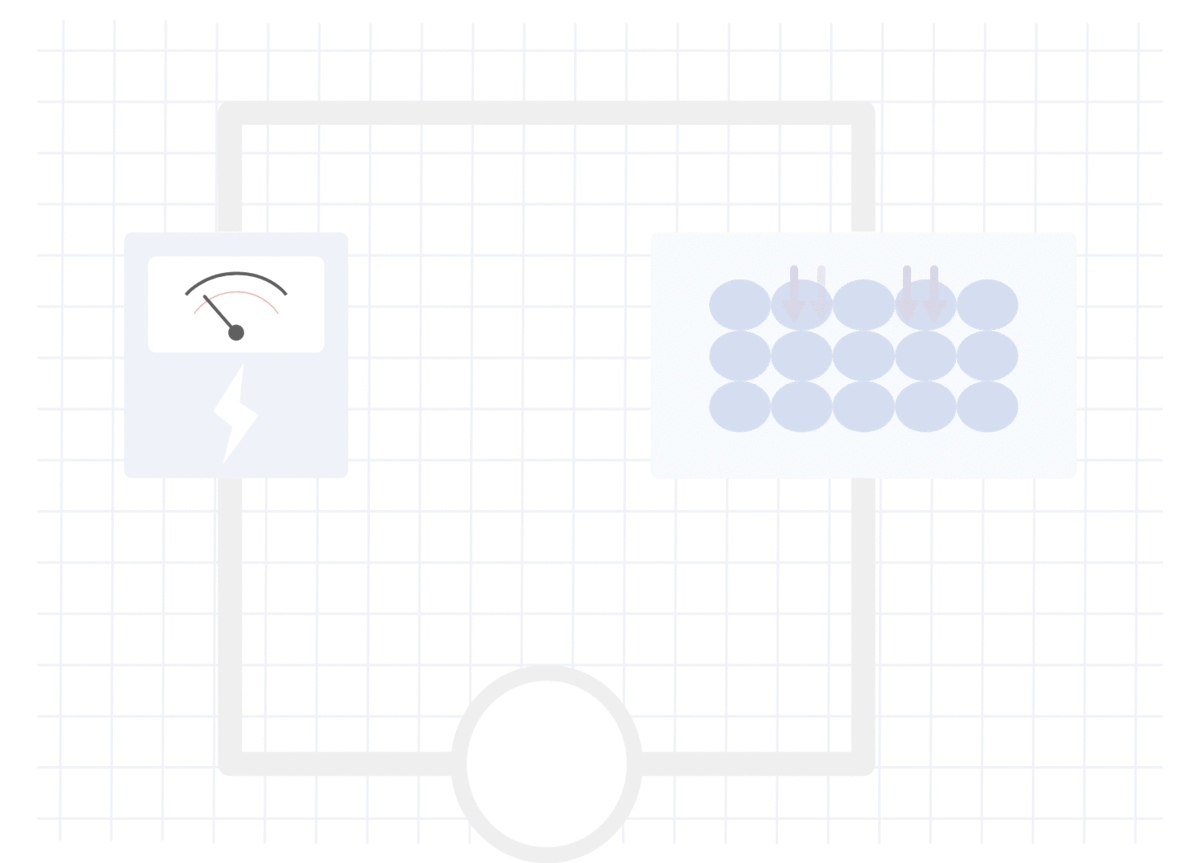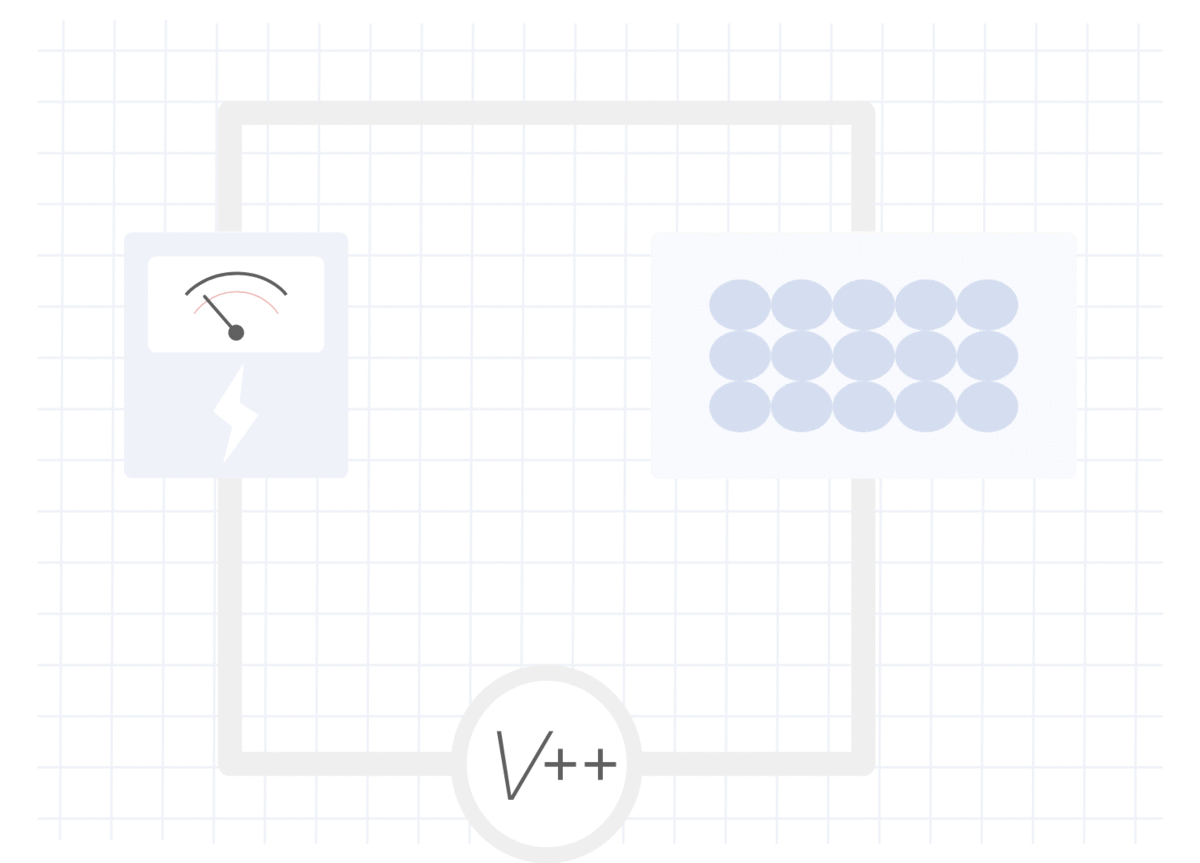
在肌肉或水中,对电流的阻力较小,因此测得的电流(V)较高,阻抗较低。
生物电阻抗分析的准确性如何?
生物电阻抗分析中使用的信号是完全安全且无痛,适用于成人和儿童, 但请注意,不建议使用生物电阻抗法用于安装心脏起搏器的人群。
一方面,许多科学出版物证明了其可靠性,精确性和准确性BIA方法在为个体提供有效的全身体水估计方面的应用。
另一方面,仍然需要对某些可能改变测试结果的因素进行标准化和达成共识。这些因素中的一些在《美国临床营养学杂志》发表的一项研究中有所描述,题为“临床特征影响生物电阻抗分析测量。”
探索更多指标:
可能影响BIA分析的因素包括:
环境
皮肤温度因测量环境的变化被认为会影响皮肤表面阻抗,正如一篇科学论文中详细描述的那样,应用生理学杂志: "控制环境温度和皮肤温度应纳入BIA测量的标准化。""
Hydration
由于肌肉主要由水组成,脱水会减少可能降低这些组织传导性的液体和电解质。因此,去脂体重更有可能被低估。水合水平在一天中变化很大,这解释了为什么一致性是准确BIA估算的重要因素。
年龄
2017年发表在身体与运动疗法杂志, "儿童和青少年通过生物电阻抗分析进行身体成分估算:系统综述", "在儿童中,基于BIA的身体成分估算与参考方法之间显示出完美的相关性。然而,儿童的去脂体重仍然经常被低估。
极度肥胖
由于解释基于总身体水分结果的无脂肪体重的方程依赖于参考人群段,对于被认为过胖的人,身体成分估计可能不准确。一项名为“内脏脂肪在重度肥胖中的评估” 表明在肥胖个体中“低估脂肪质量,且随着BMI的增加,误差变得更大。”
金属植入物
佩戴金属植入物的人可能会出现低估的体脂读数。然而,这一读数会随着时间保持不变,因此他们可以成功跟踪身体成分的变化。
不同类型的BIA设备有哪些?
许多设备多年来被设计用于以更高的准确性和便利性测量生物电阻抗。使用相同的测量方法,它们主要在电极数量以及测量身体的哪个部分与估算的哪个部分之间有所不同。
这些设备的设计之外,重要的还有用于根据接收到的频率估算总身体水分和去脂体重的算法的性质和复杂性。为了构建这些算法,科学家们使用可能会有所不同的体脂标准。
使用智能体重秤测量您的身体成分可以帮助您可靠且经济有效地跟踪变化,只要测量保持在一致水平。。
BIA 体脂秤
这些秤具有将电流从一条腿传送到另一条腿的能力。在使用之前,用户必须设置他们的年龄、身高和性别。
Handled BIA 设备
也称为手握阻抗设备,它们测量手臂和上半身的生物阻抗。
全身阻抗设备
这些常见的BIA设备由四个电极组成,每个电极放置在身体的一侧(左侧或右侧),通过手臂发送电流穿过身体并传到腿部。
DSM-BIA
The Direct Segmental Multi-Frequency BIA(或DSM-BIA)是提供生物电阻抗分析的最先进且最昂贵的设备。该设备将身体分为5个部分,并独立测量每个部分的阻抗。
生物电阻抗分析(BIA)仍然是估算成年人身体成分的一种快速且安全的方法。这就是为什么这种具有成本效益的替代方案在诊所、运动医学和其他健康相关领域被广泛使用的原因。许多研究工作尚未就一种标准达成一致,该标准可以帮助纠正使用BIA方法时的解释偏差问题。然而,测量的一致性可以准确帮助检测变化,这使得任何人都可以轻松跟踪身体成分的变化。